1 . For decades, scientists thought of the brain as the most closely guarded organ. Locked safely behind a biological barrier, away from the disorder of the rest of the body, it was broadly free of destruction of germs (病菌) and the battles started by the immune system.
Then, 20-odd years ago, some researchers began to ask a question: is the brain really so separate? The answer, according to a growing body of evidence, is no — and has important effects on both science and health care.
The list of brain conditions that have been associated with changes elsewhere in the body is long and growing. Changes in the make-up of the microorganisms resident in the gut (肠道), for example, have been linked to disorders like Parkinson’s disease. Some researchers think that certain infections could provoke Alzheimer’s disease and some could lead to emotional disorder in babies.
The effect is two-way. There is a lengthening list of symptoms (症状) not typically viewed as disorders of the nervous system in which the brain and the neural processes that connect it to the body play a large part. For example, the development of a fever is influenced by a population of neurons (神经元) that control body temperature and appetite. The effect of brain on body is underlined by the finding that stimulating a particular brain region in mice can ‘remind’ the body of previous inflammation (炎症) — and reproduce them.
These findings and others mark a complete shift in our view of the interconnectedness of brain and body, and could help us both understand and treat illness. If some brain conditions start outside the brain, then perhaps cures for them could also reach in from outside. Treatments that take effect through the digestive system, heart or other organs, for instance, would be much easier and less striking to give than those that must cross the blood-brain barrier, the brain’s first line of defence.
In the opposite direction, the effects of our emotions or mood on our capacity to recover from illness could also be used. There is an opening work under way testing whether stimulating certain areas of the brain that respond to reward and produce feelings of positivity could enhance recovery from conditions such as heart attacks. Perhaps even more exciting is the possibility that making changes to our behaviour — to reduce stress, say — could have similar benefits.
For neuroscientists, it’s time to look beyond the brain. And clinicians treating the body mustn’t assume the brain is above getting involved — its activity could be influencing a wide range of conditions, from mild infections to long-time fatness.
1. The author writes paragraph 1 mainly to ______.| A.evaluate an argument |
| B.present an assumption |
| C.summarize the structure |
| D.provide the background |
| A.Delay. | B.Cure. | C.Cause. | D.Disturb. |
| A.Treatments that cross brain-blood barrier are less used. |
| B.Previous diseases could cause the production of new ones. |
| C.Emotions could affect the capacity to fight against diseases. |
| D.Treatment of the brain takes priority over other treatments. |
I: Introduction P: Point Sp: Sub-point (次要点) C: Conclusion
A.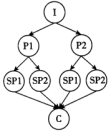 | B.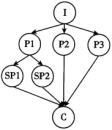 |
C.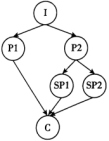 | D.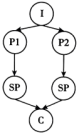 |
2 . Artificial intelligence is almost twice as accurate as a biopsy (活组织检查) at judging the aggressiveness of some cancers, experts say. Cancer kills 10 million people globally every year, according to the WHO. But for patients the disease can be prevented if detected instantly and dealt with quickly.
A recent study suggested an AI algorithm (算法) was far better than a biopsy at correctly grading the aggressiveness of sarcomas (肉瘤), a rare form of cancer. Researchers hope AI will improve outcomes for patients by giving doctors a more accurate way of grading tumours (肿瘤). Because high-grade tumours can indicate aggressive disease, the tool could help ensure those high-risk patients are identified more quickly and treated instantly. Low-risk patients could also be spared unnecessary treatments, follow-up scans and hospital visits.
Researchers say the algorithm could be applied to other types of cancer in future. The team specifically looked at retroperitoneal sarcomas, which develop at the back of the abdomen and are difficult to diagnose (诊断) and treat due to their location. They used CT scans from 170 patients with the two most common forms of retroperitoneal sarcoma — leiomyosarcoma and liposarcoma. Using data from these scans they created an AI algorithm, which was then tested on 89 patients in other countries. In grading how aggressive the tumour was, the technology was accurate in 82% of the cases, while biopsies were 44%.
AI could also recognize leiomyosarcoma and liposarcoma in 84% of sarcomas tested, while radiologists were able to identify them in 65% of the cases. Christina Messiou, the study leader, said: “We’re incredibly excited by the potential of this state-of-the-art technology, which could lead to patients having better outcomes through faster diagnosis. As patients with retroperitoneal sarcoma are routinely scanned with CT, we hope this tool will eventually be used globally, ensuring that not just specialist centres can reliably identify and grade the disease.”
Richard Davison, chief executive of Sarcoma UK, said the results looked “very promising”. He added: “People are more likely to survive sarcoma if diagnosed early. One in six people with sarcoma cancer wait more than a year to receive an accurate diagnosis, so any research that helps patients receive better treatment and support is welcome.”
1. According to the passage, AI is capable of .| A.grading the risk of sarcomas |
| B.measuring the scale of sarcomas |
| C.providing cancer treatment for clinicians |
| D.classifying cancers with its advanced algorithm |
| A.More sarcomas can be detected with the help of AI. |
| B.Biopsies will be replaced by AI algorithm in identifying cancers. |
| C.More patients suffering from cancers will benefit from AI algorithm. |
| D.AI algorithm has been applied in hospitals for detecting most cancers. |
| A.AI has a profound market in curing cancers. |
| B.New treatments for sarcomas are well underway. |
| C.AI helps identify high-risk and low-risk patients. |
| D.AI does better in assessing some types of sarcomas. |
3 . “Your mother needs a new heart,” my father told me when I called on that December afternoon. An unrelenting optimist, he spoke as if she merely needed to have a part replaced. But, although my two sisters and I knew that our mother had heart problems, this news still made us frozen for a while with our eyes widening in disbelief.
Dr. Marc Semigran of the transplant team reviewed my mother’s medical history. She’d had an irregular and rapid heartbeat for most of her life. Her present treatment — the use of a series of cardioversions, or electric jolts, to restore a normal heartbeat — would not work in the long-term. She had an enlarged and weakened heart, as well as a faulty valve.
“With medication,” Dr. Semigran said, “you have a 60 percent chance of living six months. You could have a longer life with a transplant, but there are risks. You’re at the top end of the age group of sixty years old. The lungs and other organs must be healthy and strong. While the transplant surgery is actually a straightforward procedure, acceptance by the body is the difficult thing.”
My family came together, trying to provide strength and work out what to do. We’d already gone from shock, over our mother’s condition, to worry that she wouldn’t be a suitable recipient. Despite of the risk, we chose to believe that she would make it eventually.
Word came later in December that she had been accepted into the programme. Dr. Jeremy Ruskin told us one of the reasons she had been accepted was that she had such strong family support.
One Monday in May, at about 8 p. m., my mother received a phone call from the hospital that a heart was available. As she was about to be wheeled off, my father took her face in his hands and looked into her eyes. His look said everything about their 42-year relationship.
The heart transplant operation was successful and the conditions could not have been better.
The irony of the transplant process is that one family’s loss is another’s gain; that tragedy begets fortune. It is a kind of life after death, our hearts beating beyond us. We developed a feeling of love for this new part, of gratitude for the doctors, for the process, and for those people who made a decision just for humanity.
1. How did the sisters feel to the news that their mother needed a new heart?| A.Frightened. | B.Astonished. | C.Worried. | D.Annoyed. |
| A.Her abnormal heart beat. |
| B.The age of over sixty years old. |
| C.Her willingness to the transplant. |
| D.The adaptation of the new heart in the body. |
| A.That her lungs were healthy. |
| B.That a new heart had been found. |
| C.That her family were expecting the operation. |
| D.That her family trusted the doctors' medical level. |
| A.Family support is of great importance. |
| B.Fortune favors those who are optimistic. |
| C.Confidence helps patients overcome difficulties. |
| D.Getting prepared before accepting a treatment matters. |
4 . Clinical intuition is finally getting the respect it may have long deserved. New research is supporting a process that combines rapid judgments and perceptions that occur outside of conscious awareness — a way of knowing something without knowing how you know it. The value of clinical intuition in medicine is now being studied and becoming particularly relevant as interest grows in developing AI systems that can analyze medical data to diagnose or treat patients.
A study in 2023 found that clinical intuition from physiotherapists on the prognosis for functional recovery among patients was closely associated with the recovery afterwards. Another study concluded that in comparison to relying only on clinical data, “preoperative surgeon intuition alone is an independent predictor of patient outcomes.”
“This is a cognitive process. Clinical intuition is about expertise, knowledge, and pattern recognition that accumulate through experience. The mind is putting together all kinds of information and sequencing it in ways that say this person is really sick — or not,” says Meredith Vanstone, an associate professor in McMaster University. Given the depth of this cognitive process, some experts are skeptical that AI technology can make medical decisions as well as a human physician.
“As physicians go through years of interactions with patients and seeing thousands of cases, those gut feelings become a sort of summary statement of all the experiences they’ve seen,” says Mohammad Ghassemi, a researcher at Michigan State University. “Clinicians can observe different things that are not always captured or made available by machines.”
Researchers found that physicians and nurses practicing in a medical specialty involving a high likelihood of an emergency or dimensions of complexity are more likely to use intuitive decision-making in their practice. “As surgeons, the first thing we need to do is look at the patient because the structured data may not be consistent with what we see with the patient,” says Gabriel Brat from Harvard Medical School.
Research has found that clinical intuition from nurses and physicians about the chances that older patients visiting emergency departments would die or have other adverse outcomes within 30 days was highly accurate.
None of known experiences suggest that clinical intuition should be blindly acted upon. Making clinical decisions solely on the basis of a physician’s intuition isn’t the way to go, experts say. But relying solely on medical algorithms (mathematical models) that generate predictions about how a patient is likely to respond to different treatments isn’t the best course of action either.
To optimize patient care, some experts believe a hybrid approach that integrates clinical intuition, predictive algorithms, patient preferences, and other key factors is essential.
1. According to the passage, clinical intuition is influenced by ________.| A.rapid judgement |
| B.medical algorithms |
| C.conscious awareness |
| D.professional knowledge |
| A.Clinicians have a sharp eye for a patient’s condition. |
| B.Machines always generate more accurate predictions. |
| C.Doctors should summarize the experiences they’ve seen. |
| D.Physicians’ interactions with patients have been devalued. |
| A.To introduce the wide use of clinical intuition. |
| B.To explain the logic chain of clinical intuition. |
| C.To prove the accuracy of clinical intuition. |
| D.To present feedbacks on clinical intuition. |
Susana Vazquez-Torres is a fourth-year graduate student at the University of Washington who wants to someday invent new drugs
Lately, she
Part of the problem is
6 . A quick increase of dopamine (多巴胺) shifts mice into a dreamy stage of sleep. In the mice’s brains, the chemical messenger triggers rapid-eye-movement sleep, or REM, researchers report in the March 4 Science.
These new results are some of the first to show a trigger for the shifts. Understanding these transitions in more detail could ultimately point to ways to treat sleep disorders in people.
Certain nerve cells in the ventral tegmental area of the mouse brain can pump out dopamine, a molecule that has been linked to pleasure, movement and learning, which is then delivered dopamine to the amygdalae, two almond-shaped structures deep in the brain that are closely tied to emotions.
Using a molecular sensor that can tell exactly when and where dopamine is released, the researchers saw that dopamine levels rose in the amygdalae just before mice shifted from non-REM sleep to REM sleep.
Next, the researchers forced the mice into the REM phase by controlling those dopamine-producing nerve cells using lasers and genetic techniques. Compelled with light, the nerve cells released dopamine in the amygdalae while mice were in non-REM sleep. The mice then shifted into REM sleep sooner than they typically did, after an average of about two minutes compared with about eight minutes for mice that weren’t prompted to release dopamine. Stimulating these cells every half hour increased the mice’s total amount of REM sleep.
Additional experiments suggest that these dopamine-making nerve cells may also be involved in aspects of narcolepsy (嗜睡症). A sudden loss of muscle tone, called cataplexy, shares features with REM sleep and can accompany narcolepsy. Stimulating these dopamine-making nerve cells while mice were awake caused the mice to stop moving and fall directly into REM sleep.
The results help clarify a trigger for REM in mice; whether a similar thing happens in people isn’t known. Earlier studies have found that nerve cells in people’s amygdalae are active during REM sleep.
Many questions remain. Drugs that change dopamine levels in people don’t seem to have big effects on REM sleep and cataplexy. But these drugs affect the whole brain, and it’s possible that they are just not selective enough.
1. What can we learn from this passage?| A.People with sleep disorders could benefit from the research. |
| B.Dopamine is generated in two almond-shaped structures. |
| C.Dopamine levels rose after mice shifted to REM sleep. |
| D.An increase of dopamine can trigger REM in people. |
| A.the entire brain |
| B.REM sleep and cataplexy |
| C.drugs affecting dopamine levels |
| D.people suffering from sleep disorders |
| A.To introduce two stages of sleep of all animals. |
| B.To explain dopamine as a trigger for REM in mice. |
| C.To present a new way to cure sleep disorders in people. |
| D.To propose a pioneer research interest in brain structure. |
Cholera used to be one of the most
Tuyouyou was chosen as a researcher of a team of scientists
At the Nobel Prize Lecture on 7 December, 2015,
Speaking of medicine, through new technology, people who have brain
10 . In the 1770s, an English doctor called Edward Jenner gave his gardener’s son cowpox (牛痘) and then deliberately infected him with smallpox (天花) to test his assumption that people who were frequently exposed to cowpox, a similar but less severe virus, would avoid catching smallpox. It worked and cowpox as the vaccine (疫苗) was highly effective. “Vaccination”, from the Latin word for cow, soon became commonplace.
Challenge trials are forms of research where, rather than relying on data from natural infections, we intentionally expose someone to a disease in order to test the effectiveness of a vaccine or treatment. Things have changed a lot since Jenner’s time, of course, when it was not uncommon for doctors to conduct this kind of research. Even so, there’s the continuous sense that there’s something immoral about making someone ill on purpose.
But this shouldn’t blind us to the extraordinary power of challenge trials. They could become increasingly important weapons in the medical research, in a situation where vaccine technology is advancing and the threat of diseases jumping from animals into human beings is increasing.
Much has been done to reduce the risks of challenge trials. Like respiratory syncytial virus (RSV), researchers have involved adults who are at a low risk of severe illness. These acts have already cut down a massive range of vaccine candidates. With their help, the world will soon have the first vaccines against RSV, which kills tens of thousands of newborn babies each year. But not all diseases are like these ones. We don’t always know the dangers volunteers might face; we don’t always have treatments ready. What then?
We could, of course, just avoid these questions entirely, and rely on other types of research.But that doesn’t always work: sometimes, animal testing is tricky and uninformative, because the disease doesn‘t develop in the same way as it would in humans. In contrast, challenge trials can be deeply informative within weeks, with far fewer volunteers. And the benefits can be surprisingly high. Take the latest pandemic. At the end of last year, as the number of deaths is estimated to have reached about 17.8 million, it’s also estimated that 20 million had been saved by vaccines.In the years to come, they will hopefully save millions more.
In order to make sure we are as protected as possible from current and future threats, we should try to get rid of the misbelief in challenge trials, making them a more familiar part of our tool kits. Perhaps the greatest reward of all would be to make sure participants’ efforts are worthwhile: by designing trials to be fair and effective and applying them when and where they might make a real difference. In short, by helping them to save thousands, if not millions of lives.
1. The author tells the story of Edward Jenner mainly to______.| A.give a definition of challenge trials |
| B.introduce the topic of challenge trials |
| C.highlight the effectiveness of his vaccine |
| D.explain the origin of the word “vaccination” |
| A.The issues behind challenge trials can be solved. |
| B.The dangers of challenge trials outweigh the benefits they bring. |
| C.Challenge trials can benefit numerous lives in spite of their risks. |
| D.Challenge trials can set back the development of vaccine technologies. |
| A.People should still be careful about challenge trials. |
| B.A more open attitude should be taken towards challenge trials. |
| C.Challenge trials guarantee participants protection against threats. |
| D.More volunteers involved can improve the accuracy of challenge trials. |
| A.Should we use challenge trials to find cures? |
| B.Can challenge trials be a block to medical progress? |
| C.Can challenge trials be the end of infectious diseases? |
| D.Should we replace animal testing with challenge trials? |



